Early intervention can mean a range of different things to different people. In the context of workplace rehabilitation, the best approach to early intervention is prevention of injury through implementing best practices to ensure the physical and mental health safety of everyone in the workplace.
However, in the context of the facilitated conversation service, early intervention refers to a fast and proactive approach following a work injury claim. The purpose of the service is to re-establish a positive relationship between the injured worker and their employer, and minimise the risks for both parties. Data has indicated that the quicker the communication is re-established, the better the return to work outcomes. This service can be utilised for early intervention prior to the claim being determined, as it can be an effective way to resolve the issues and implement a return to work before a decision is made.
Ideally a referral for facilitated conversation will occur within the first 6 weeks of the issues arising between the injured worker and their employer. In many situations this may be in the first 6 weeks of the injury claim, however it can also occur later in the claim where relationship or interpersonal issues occur between the injured worker and their employer during the return to work process. Where it is not possible to commence this process within the first 6 weeks of the issues arising, later referrals can be made, however it is best to discuss the specific situation with the coach to determine if facilitated conversation is the most appropriate approach.
The purpose of the facilitated conversation is to assist the worker and their employer to engage in open and honest communication with each other, clarify issues, brainstorm and discuss a range of options for resolution and then agree on an action plan together. The earlier this process is commenced, the better the opportunity to gain a positive outcome for everyone involved. Where issues have been ongoing for 6 months or more, it may be more appropriate for the participants to be provided with a more formal mediation service to assist them to move forward together.

Recently I read the first “self-improvement” book that has genuinely led to me changing my habits. Atomic Habits by James Clear provides a very simple and practical way to develop good habits (or unlearn bad habits) that can snowball into great achievements and lifestyle changes. He clearly demonstrates how many great achievers get there through the compounding of tiny changes. After the first chapter I noticed the same transient excitement that I often get when I read any “self-improvement” book, but then Atomic Habits introduces a simple and practical model to take that excitement and start making tiny changes after only the second chapter. The one aspect from the introductory chapter that particularly resonated with me was the concept that for a habit to stick it must be in line with our perceived or intended “identity”. An example given is that “the goal is not to read a book, the goal is to become a reader”. If you take on this identity of being a reader then the motivations become much more intrinsic, you naturally ask yourself “is this what a reader would do?”
I will attempt to summarise Clear’s model, but I whole-heartedly recommend reading the book to get the full effect.
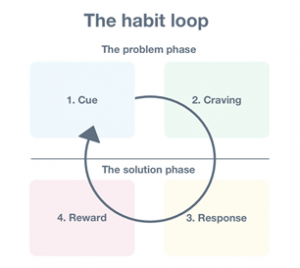
The whole model is based around four stages the mind and body go through when a habit is being developed (usually an entirely unconscious process).
Stage 1: Cue – a piece of information that reminds you of a potential reward (eg. you see your fridge)
Stage 2: Craving – the mind/body motivation for the reward (eg. you get excited by the thought of food)
Stage 3: Response – the action/habit (eg. looking in the fridge and grabbing a snack)
Stage 4: Reward – satisfying the craving (eg. eating the snack)
Here is how the model uses these four stages for intentional habit-building, and how I started to apply each element to help me do exercise after work rather than flopping on the couch and struggling to get the motivation to get back off the couch. The model also works in the opposite way to unlearn bad habits.
Overall identity: a fit and disciplined person
Stage 1 (cue): Make the cue for your intended habit obvious (I used Clear’s “habit stacking” method by identifying a habit I already have – taking off my work shoes – to be the cue for putting on my activewear; an obvious cue for exercising).
Stage 2 (craving): Make the intended habit attractive (Clear explains how our bodies crave an immediate response, so thinking about the final goal such as running a marathon will not elicit an internal craving for the habit. For my exercise habit I am using Clear’s example of thinking about the immediate after-effects of exercising, thereby developing a craving for the exercise-high).
Stage 3 (response): Make the intended habit easy (I am only committing to 5 minutes of walking/running/yoga and even if I stop then, it will still contribute to the repetition required to solidify the habit – as you could guess I have always continued after 5 minutes since the hard work of getting going is already done).
Stage 4 (reward): Make the intended habit satisfying (I take a moment to revel in the exercise high, allow myself the slow walk cool down, feeling high and mighty, and grant myself the guilt-free evening on the couch).
Some of the elements may seem like common sense but often we miss one part, and it is the one thing that leads to a failure to keep up with new habits. I encourage you to try applying the model to a habit you would like to develop and see if there is something missing. Happy habit-forming!

If you’re currently in a rehabilitation program to recover from an injury, you may be starting to think about how to keep your progress going over the Christmas break. For various reasons it may be hard to access your usual programs over Christmas, either because of business closures or because of personal travel during this time.
Here are some tips to ensure you keep improving your strength and fitness over the Christmas break:
- Ask your providers now whether they will close over Christmas and how long they will be closed for.
- Talk to your physio / exercise physiologist about an exercise program you can do at home to keep your progress going through the break. Think of what would be the best way for you to remember the exercises – you could write them down or even film them on your phone.
- If you usually do weights at the gym and don’t have access to these at home, you can substitute various sized bottles and fill with water – 1L water = 1 kg.
- Simply stay active! While specific exercises targeted at your injury are useful, a lot of research has found non-specific exercise to be effective in rehabilitation and pain reduction. This involves activities that incorporate the full body such as walking, hiking, running, cycling, swimming, dance, boxing, circuit classes, Pilates, the list is endless. Do approach this with caution, for example you may not want to do boxing three weeks after a shoulder surgery, but instead going for regular walks could provide some light movement to prevent shoulder pain and stiffness. Discuss with your health provider what some safe general exercise options could be for you!
- If you are usually doing a hydrotherapy program and your hydro pool has closed, you may be able to access other pools that are open through this time to do a modified program on your own. Ask your hydro provider to help you put together a program you can do independently.
- Set a reminder on your phone/calendar to remind you to do your exercises regularly if your routine is changed over Christmas.
- Have a family member or friend either join you or keep you accountable – tell them specifically what exercise(s) you intend to do and how often.
Do what you can but also don’t forget to chill out, have some fun, spend some quality time with friends and family, and schedule some me-time. You’re allowed to let your rehab slip a little for a week or two and come back refreshed, just be ready to ease back into it in the New Year – taking that one step back at first will have you moving forward much sooner.

If you are thinking “awesome, I finally have the perfect ergonomic position at my workstation; my eyes line up with the top of the monitor, I’ve got my lumbar support chair, my hips are at a comfortable 90 degrees, my feet are propped up to the exact right height, now I mustn’t budge from this position,” then you may need to adjust priorities.
Something we emphasise with our office-worker clients is that while ergonomic set-up is certainly helpful, the most important tool to prevent sedentary work injury is to move. Often that stiffness in your neck or back when you wake up in the morning isn’t because you slept wrong, or your desk isn’t set up right, it is most likely because you did not move enough the previous day.
Here are some tips to fit movement into your day:
- Set a timer for every 15 minutes to do some sort of movement (you can cycle between quick neck stretches, a few sit-to-stand movements, walking… listen to your body)
- Many people have trouble doing the above as they want to “get stuck into” a task for a longer period without distractions. This is fine, instead you can compensate by taking longer movement breaks when you finish tasks.
- Another alternative to a timer is connecting movement to daily habits that you have already developed such as getting a coffee, going to the bathroom, or collecting printing. Every time you do one of these habitual tasks, let that be a reminder to do a quick movement for instance:
- 10 squats
- 20 heel raises
- 15 wall push-ups
- Walk up and down a staircase
- Have a small cup of drinking water so that you need to walk to fill it up frequently
- Choose to use a bathroom that is the furthest from your desk
- Use the stairs whenever you can
- If you have a sit to stand desk, change from sitting to standing (or vice versa) every hour
- Take standing/walking meetings
- Give your colleague a message in person rather than sending an email
- See our Facebook page for some simple stretches to break up your day
- Smart watches have great apps to remind you to move
- Go for a walk at lunch time – even 5 minutes makes a difference!
It will take time to develop these habits. Try adding one or two of these movements to your day, and when they have become habitual, then you can try adding more. Time should not be a barrier to beginning a movement habit, once these become integrated into your day you should find that you will become more alert and efficient in your other tasks.

Now that the risk of Covid-19 has reduced dramatically in South Australia, Adaptive Workplace Solutions have resumed face to face appointments with clients.
However, we are still taking the threat of coronavirus extremely seriously and have made a range of changes to our practices to ensure the ongoing safety and protection of our clients and staff.
Steps we have taken to ensure safety of all parties include:
- Complying with 4 square metre rule – only one person per 4 square metres of each room/building. We have calculated the square metres of each meeting room and have put up signage to ensure that we do not exceed this limit.
- Social distancing – tables and desks have been moved in each meeting room to ensure that clients and staff do not sit closer than 1.5 metres during appointments.
- Hand sanitising stations – we have purchased high quality hand sanitiser that is readily available in all of our offices for clients and staff members to use regularly.
- Disinfecting of office spaces – tables, chairs, computer equipment, benches, doorhandles, etc are wiped down with high grade disinfectant between each client. Staff are restricted to using one work area per day, with the area thoroughly cleaned each afternoon/morning.
- Contact tracing – we are collecting details from each client who visits our offices that can be used to inform the relevant health authorities in the unlikely event of a covid-19 case on our premises.
- Information provided to clients and staff – we have collected information from SA Health and from the Australian Government and are providing this to clients on arrival. Information is also displayed via posters on the walls of our offices and buildings. A clear Covid-19 safety plan has been drafted for staff and is under continual review as new advice is provided by the Government.
- Staff are instructed not to attend the office if they have any cold/flu or respiratory symptoms and clients are contacted the day before their appointment to remind them not to attend if they have any relevant symptoms. In the event that either the consultant or the client have symptoms, their appointment will be changed to a phone or video appointment.
- We are still offering telehealth appointments via Zoom video or phone for clients that are not comfortable to attend face to face appointments at this stage. We are also doing group meetings such as case conferences or medical reviews via telehealth to ensure the social distancing requirements are met.
If you have any questions about the safety of attending appointments in our offices, or would like to discuss our approach to the Covid-19 pandemic, please don’t hesitate to contact one of our friendly staff members.
Adaptive Workplace Solutions can now offer Psychology Services!


Kelly and Kate have both achieved their Provisional Psychologist Registration, meaning they can now both offer:
- Psychological Treatment Services
- Psychological Worksite Assessments
- Vocational Assessments
This is an exciting new phase for Adaptive Workplace Solutions as we broaden our service provision to ensure the most effective services are available to both our clients and our referrers.
Congratulations to both Kelly and Kate – what wonderful achievements!!

This research project sought to provide Australian research on the Progressive Goal Attainment Program (PGAP). The PGAP aims to reduce the impact of four psychosocial risk factors known to be associated with work related disability. The psychosocial risk factors included are perceptions of injustice, catastrophic thinking, fear of activities associated with the persons condition and perceived levels of disability. The research project aimed to provide an evaluation of the PGAP on two levels. How effective is the program at reducing the four psychosocial risk factors associated with work related disability and does participating in the PGAP improve the persons readiness to return to work?
To answer these questions, we contacted 29 people who had been referred to Adaptive Workplace Solutions as a result of a work-related injury or condition. Of those contacted 20 provided consent to participate in the research and their results from the PGAP were gathered to analyse the effectiveness of the program. Each persons’ file was reviewed, and they were allocated a work readiness score at referral and upon completion of the program.
The results of the research project demonstrated that the PGAP was effective in reducing the identified psychosocial risk factors associated with prolonged absence from the workforce and increased work disability. This result was consistent with the international research on the PGAP. The other aim of the study was to assess the improvement’s in work readiness following participation in the PGAP. The data indicated that 75% of people who had participated in the PGAP had an improvement in return to work readiness. The other interesting finding was that people who experienced improvements in two or more of the psychosocial risk factors were more likely to also experience improved return to work readiness scores. In summary, the results support the inclusion of the PGAP in work injury rehabilitation where people are at risk of experiencing psychosocial risk factors associated with return to work.

What do I need to know about sleep?
Sleep is a natural process that allows the brain and body to rest and recover. When you are asleep, your eyes are closed, most of your muscles are relaxed, and your consciousness is practically suspended. But while your body is still, your brain is quite active.
Sleep is important as it helps us restore and recover ourselves physically while also assisting us to organise things in our brain. People need sleep in order to function well – mentally and physically.
Going without sleep or having insufficient sleep can lead to a range of issues including:
• Poor mood / feelings of depression
• Lack of concentration
• Irritability
• Low motivation
• Heart disease
• Blood pressure
• Diabetes
• Increased likelihood of road accidents or workplace accidents
Sleep can be affected by a range of things including ageing, lifestyle commitments, injury, trauma, stressors, health problems, anxiety, depression, medication.
However a regular sleep pattern CAN be re-established after a disruption, even a significant disruption.
Sleep cycle
Sleep occurs in cycles that last around 90 minutes per cycle. During each cycle, different types of brain activity occur.
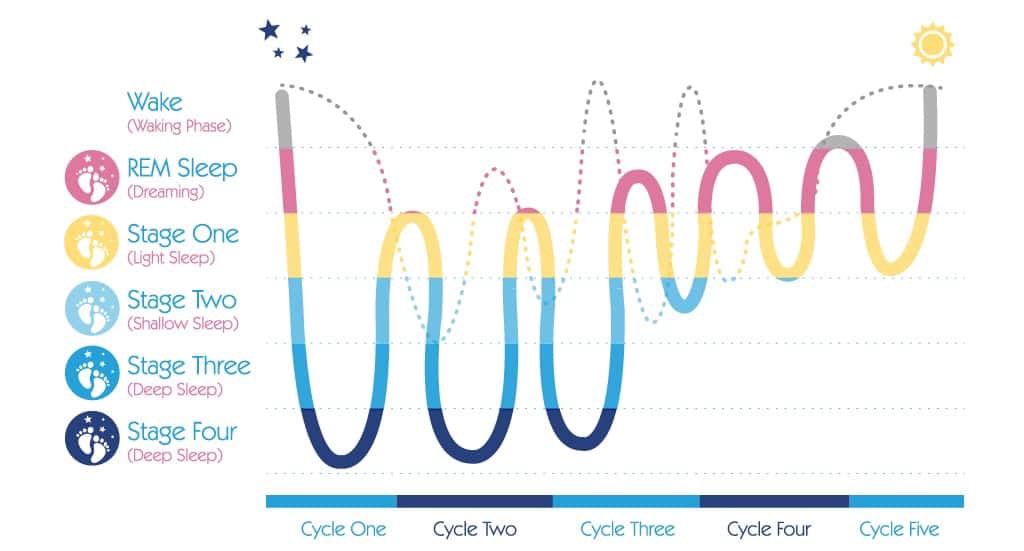
5 stages of sleep have been identified based on this brainwave activity:
Stage 1: Drowsiness. This is often referred to as the transition between awake and asleep. The eyes are generally closed, but the person awakens easily. If disrupted during this period, people will often state that they were not yet asleep or were just resting. This usually lasts for around 5-10 minutes
Stage 2: Light sleep. This sleep stage involves spontaneous periods of muscle activity mixed with periods of muscle relaxation. The heart rate slows and body temperature decreases. The body prepares to enter deep sleep.
Stages 3 and 4: Deep Sleep. Also known as slow-wave or delta sleep. During these stages the breathing is more relaxed, heart rate slows, sound and light sensitivity diminish. It is difficult to wake someone while in a deep sleep. Quality sleep needs to include deep sleep. Often when people seem to have had sufficient sleep (as measured by hours of sleep) but are still tired and fatigued each morning, it may be that they are not achieving deep sleep in their cycle. This deep sleep is vital in the secretion of the growth hormone. This hormone is necessary to restore the body and if this does not occur, people can be more prone to infections and disease. Alcohol, medication and stress can all impact on your ability to achieve deep sleep.
Stage 5: REM (Rapid Eye Movement) sleep. Also known as dream sleep. During REM sleep there is heightened brain activity, but the mind paralyses the muscles, possibly to keep the body from acting out the dreams and harming itself. The first period of REM typically lasts around 1 minutes, with each recurring REM stage becoming longer. The final stage may last around an hour. REM sleep is vital for normalising cognitive and emotional activities.
How much sleep do we need?
Different people require different amounts of sleep, which changes over a person’s life span. The average for an adult is around 7-8 hours, but anything within 5–10 hours can be normal.
The best guide to whether you are having enough sleep is how you function throughout the day. If you are sleepy and struggle to concentrate it is likely you are not getting enough sleep.
The first 3-5 hours of sleep is when the deepest sleep occurs (see graph above). This is the most restorative.
Waking up a few times during the night is quite normal and nothing to be concerned about. This usually occurs during the periods of light or REM sleep spaced out over the night. Being concerned or worried about waking up generally increases the likelihood of it being difficult to get back to sleep and increase these awake periods.
Sleep deprivation Scale
The Epworth Sleepiness Scale (ESS) can provide a measure of the impact of sleep deprivation on daytime function. This should only be used by people not on sleep medication.
If you feel you may be deprived of sleep and are not taking any sleep medication, completing this quick scale can give you an indication of how much impact it is having on your life:
0 would never doze
1 slight chance of dozing
2 moderate chance of dozing
3 high chance of dozing
Situation Rating
Sitting and reading ______
Watching TV ______
Sitting inactive in a public place (e.g. movie or meeting) ______
Passenger in a car for 1 hour with no break ______
Lying down in the afternoon when circumstances permit ______
Sitting and talking to someone ______
Sitting quietly after a lunch without alcohol ______
In a car, while stopped for a few minutes in traffic ______
TOTAL ______
Score indicator:
0-4 Satisfactory daytime functioning
5-9 Daytime tiredness, lack of energy
>10 Excessive daytime sleepiness
Sleep Diary
If you feel you have an issue with sleep or score 5 or above on the Epworth scale, the first step in making change can be to record relevant information in a sleep diary for 4-5 days in a row. This should give a clear indication of a baseline pattern and can identify potential problem areas and solutions.
Each day record:
• any daytime naps and their duration
• number of cups of tea, coffee, cola or energy drinks and approx. time each one was consumed
• number of standard drinks of alcohol and approx. time of consumption
• any sleep medication and time taken
• time when you go to bed
• approx. time when you fall asleep
• number of times you wake through the night and approx. indication of how long you were awake for
• time when you wake
• time when you got out of bed
It is important not to be too obsessed with clock watching or it will interfere with your natural pattern. This is particularly the case when waking in the night – clock watching will only increase the time you are awake for. An estimate of your sleep behaviours is fine.
Creating Positive Change
People who are having difficulties with sleep during the night often try to go to bed earlier or stay in bed longer to “catch up” on their sleep. This generally makes the problem worse, as more time is spent lying in bed awake. Often people feel anxious or frustrated about not sleeping during this time, which can build up an association between being in bed and negative emotions.
It is not necessarily easy to re-set your sleep pattern. It needs commitment and persistence. Initially you are likely to feel tired and irritable and may even get less sleep as your body adjusts to a new pattern. You will often feel more tired during the day, but it is important not to nap until the pattern is established.
Be aware it may take from 4-6 weeks to notice any improvement – repetition and consistency is key.
Effective Strategies:
• The most effective strategy when re-introducing a sleep pattern is ensuring a regular wake-up time. Stick to this wake-up time 7 days per week, even if you feel you haven’t had much sleep during the night.
• Get sunlight within 10-15 minutes of waking if possible.
• Only go to bed when you feel sleepy rather than at a fixed time in the evening.
• Establish a regular evening sleep routine – this is a pattern of behaviour that tells your body and mind it is time to go to sleep.
• Only stay in bed if you are sleeping. If you are lying in bed awake for more than 20 minutes, get up and do something relaxing in another room until you feel tired again.
• Only use the bed/bedroom for sleep or sexual intimacy. Avoid laying in the bed to rest during the day or using the bedroom to watch TV, eat, smoke, work, play computer games or chat on your phone.
• Avoid taking daytime naps.
During the Day:
• Keep a regular routine for meals, medication and general daily activities
• Pace your activities throughout your day
• Spend time outdoors in the afternoon if possible
• Avoid napping
• Keep as active as possible
• Reduce coffee to no more than 3 cups per day
During the evening:
• Relax and prepare for sleep
• Utilise an hour of quiet activity before you intend to sleep
• List what is on your mind and organise to do it tomorrow (to avoid worrying or planning throughout the night)
• Learn and use a relaxation tool to switch off. This may be a breathing exercise, mindfulness, meditation, or something that works for you.
• Avoid exercise late in the evening – light exercises early in the evening can be helpful
• Avoid caffeine for at least 5 hours before bedtime
• Avoid smoking before bedtime and during wakening
• Avoid alcohol near bedtime
• Avoid a heavy meal too close to bedtime
• Reduce disturbing noises and be calm about the unavoidable
• Avoid screentime – particularly laptops and mobile phones for one hour before bed
At bedtime:
• Develop a bedtime routine and follow it every night
• Recognise any emotional responses for what they are and use appropriate coping techniques to deal with such responses
• Only go to bed when you feel ‘sleepy tired’, not when you are just physically exhausted or you think its time for bed
• Keep reading and TV for another room
• Avoid using your bed for anything other than sleep or sexual intimacy
• Do not lie in bed awake for longer than 15-20 minutes
• During that 15-20 minutes enjoy relaxing in bed if you do not fall straight to sleep
• Use relaxation techniques to induce sleep
• Prepare somewhere to go (e.g. another room) and something to do if you do have to get up
• Return to bed only when you feel sleepy again
• Repeat the rising routine as frequently as necessary
• Keep the bedroom dark
When getting up in the morning:
• Get up at the same time each morning
• Have a routine that refreshes and takes your needs into account
• Allow time to avoid demanding morning routines
• Make a plan for the day
• Ensure that you have at least one rewarding activity.
Important tips when trying these strategies:
• Rather than being discouraged if there are lots of things you have identified that you can change, be pleased that you have identified a number of things that can help as this increases your chance for improvement.
• Don’t expect to have great results overnight – improvement may take 4-6 weeks.
• Change can take longer if the reasons for the sleep disruption are more complex. Be patient with yourself and take things one step at a time.
• It can be helpful in the initial stages to focus on behaviours/strategies you can ADD rather than things you need to avoid or stop doing.
• Feeling tired throughout this process of change is totally normal – feeling sleepy during the day is often one of the last things to disappear.
• A habit is learned and established by consistent repetition over long periods of time – it might be hard, but don’t give up!
SUMMARY: Tips to Sleep Better
• Stick to a consistent wake up time – even on the weekends. This helps to regulate your body’s clock and could help you fall asleep and stay asleep for the night.
• Practice a relaxing bedtime ritual. A relaxing routine activity right before bedtime conducted away from bright lights helps separate your sleep time from activities that can cause excitement, stress or anxiety.
• Avoid daytime naps – particularly in the afternoon. Power napping may help you get through the day, but if you find that you can’t fall asleep at bedtime, eliminating even short catnaps may help.
• Exercise daily. Vigorous exercise is best, but even light exercise is better than no activity. Exercise at any time of day, but it is best to avoid vigorous exercise for a few hours before bedtime.
• Avoid alcohol, caffeine, cigarettes and heavy meals in the evening. You may feel that alcohol or heavy meals make you tired enough to fall asleep, but these can interrupt with the natural sleep cycle and may lead to waking early or not getting sufficient deep sleep.
• Wind down – Your body needs time to shift into sleep mode, so spend the last hour before bed doing a calming activity such as reading, talking, or listening to music. For some people using an electronic device such as a laptop or phone can make I hard to fall asleep because the particular type of light coming from the screens is activating to the brain. If there are any activities that you associate with anxiety about sleeping, remove them from your bedtime routine.
• Evaluate your room. Design your sleep environment to establish the conditions you need for sleep. Your bedroom should be on the cooler side (around 15-19 degrees). It should also be free from any noise and light that can disturb your sleep. If you have environmental distractions you can’t remove, try using eye shades, ear plugs, white noise machines, or other devices.
• Sleep on a comfortable mattress and pillows – Make sure your mattress and pillow is comfortable and supportive.
• If you can’t sleep, don’t just lay there – go into another room and do something relaxing until you feel tired.
• Use your bed only for sleep and sex to strengthen the association between bed and sleep.
Our Rehabilitation Counsellors can help you to implement these strategies and improve your sleep health. Contact us today for more information if you need additional assistance.

We were all very excited to move into our new head office in Plympton Park last week. This has been a big project for 2019, as we had outgrown our previous premises and involved the complete renovation of what was previously a home into a functional and purpose built Adaptive Workplace Solutions office space. We had our first team meeting in the new office on Tuesday the 22nd of October and officially moved in on the 23rd.

On Friday we surprised Kelly with a baby shower in the new building which was a lot of fun and enjoyed by all who attended.

We can’t wait to finish off all the final details in our new office space and continue to renovate the outdoor areas. We look forward to having future meetings in this new facility which is large enough to host both small and large meetings with clients, case managers, employers and treatment providers.

Your resume is a tool which provides a first impression to a prospective employer. It is important to ensure that the impression they get is as positive and impressive as it can possibly be, so that they want to find out more by inviting you in for an interview.

Your resume says a lot about you, and may say more than you realise. Some of the things you may not know that you are telling a prospective employer include:
1. How well you have researched current job searching practices.
If your resume starts off with an objective statement, or lists personal information that is not relevant to the role (e.g. date of birth or marital status), it is telling your potential employer that you have not bothered to do your homework on currently acceptable protocol and trends. Ensuring that all information provided is relevant and professional speaks volumes towards helping you make the best possible first impression.
2. Your ability to concisely summarise information.
With regards to your Resume, less is definitely more. It can be tempting to try and pad out your Resume with heaps of details in an attempt to make it look more impressive, but this can actually detract from your first impression and increases the likelihood that they may not even bother to read it. It is important to be as concise as possible. The current expectation for resumes is no longer than two pages, regardless of the length of your career. It may be daunting to try and summarise your achievements within two pages, but avoid the temptation to go over that limit. Exceptions may be made for curriculum vitaes if you are in the medical or academic profession, but the rest of us have to keep it brief. Concisely communicating information is a critical component of many jobs, so it is your best interest to showcase this ability in your resume. It may help to limit your listed experience to the last ten years, or twenty at the very most.
3. Your ability to use correct spelling and grammar.
Confusing to, too and two or your and you’re is increasingly common in today’s autocorrect society but your resume is one place to make sure you are perfect. Typos or grammatical errors in your resume can cost you the opportunity for interview. Don’t just rely on your spell check, read it, re-read it, have a friend read it and then read it backwards to make sure there are no mistakes on your resume.
4. Your computer skills.
A prospective employer often wants to know that you know your way around word processing software. Ensure that your margins are aligned, spaces are uniform, consistent font is used throughout your Resume and that it all looks neat and easy to read. This will also ensure that important information is easy to find – the average time that an employer will view your Resume for is 6 seconds! It is important to make sure that the important information is clear and easy to find. Good formatting will assist with this.
5. Your attention to detail.
While you may list “attention to detail” as one of your key attributes within the content of your Resume, inaccurate dates or missing information may indicate that this is not in fact the case. Ensure all of the key details are accurate and included – it is more important than you might think. Getting a critical friend to help you edit can be useful in picking up missing information.
6. How seriously you take yourself and this potential job.
If your resume looks slapped together, with little forethought, it sends the message that this job isn’t that important to you, whether that’s true or not. No matter what the time pressure, take the time to create a professional-looking, contemporary, accurate and up-to-date resume. Always include up-to-date referee contact details rather than writing “referee details can be provided upon request” as this may look like you are either trying to hide something or haven’t taken the time to organise a reference before sending in your application.







